Restoring Your Stride: Foot and Ankle Surgery Options for Medical Tourists
Our feet and ankles are the foundation that carries us throughout life. They propel us forward during walks, runs, and adventures, allowing us to explore the world confidently. However, for many Americans, foot and ankle pain caused by injuries, arthritis, or chronic conditions like plantar fasciitis can significantly limit mobility and enjoyment of daily activities. Thankfully, foot and ankle surgery offers a solution to restore function and get you back on your feet, literally and figuratively.

Surgical Solutions for a Pain-Free Step Forward
Medical tourism allows access to high-quality foot and ankle surgery at a fraction of the typical US cost. Here’s a closer look at some of the most common procedures offered by medical tourism destinations:
Bunions: Minimally invasive bunionectomy procedures can correct the misalignment of the big toe joint, alleviating pain and pressure on the bunion bump. This can significantly improve comfort and allow you to wear shoes without discomfort.
Hammertoes: Surgical correction of hammertoes addresses the abnormal bending of the middle toes, often caused by tight shoes or heredity. This can improve the appearance and function of your toes, reduce pain, and prevent further complications.
Plantar Fasciitis Surgery: In severe cases of plantar fasciitis, a chronic inflammation of the plantar fascia tissue in the foot, surgical intervention may be necessary. This can involve minimally invasive procedures to release tension in the fascia and promote healing.
Ankle Reconstruction: For complex ankle injuries or instability, reconstructive surgery can repair ligaments, tendons, or fractures to restore stability and function in the ankle joint. This can be crucial for athletes or individuals who require a high level of ankle mobility.
By understanding these procedures and prioritizing quality care abroad, you can confidently take the first step toward a more active and pain-free future. Medical tourism offers a path towards reclaiming your mobility and getting you back to enjoying life on your own two feet.
Bunions
Our feet are the unsung heroes that carry us throughout our lives. They provide the foundation for balance and mobility, allowing us to explore the world with each step. But for many Americans, bunions – the bony bumps that form at the base of the big toe – can cause significant pain and discomfort, hindering our ability to walk, run, and participate in activities we enjoy. Thankfully, minimally invasive bunionectomy surgery offers a solution to restore pain-free movement and get you back on your feet with confidence.
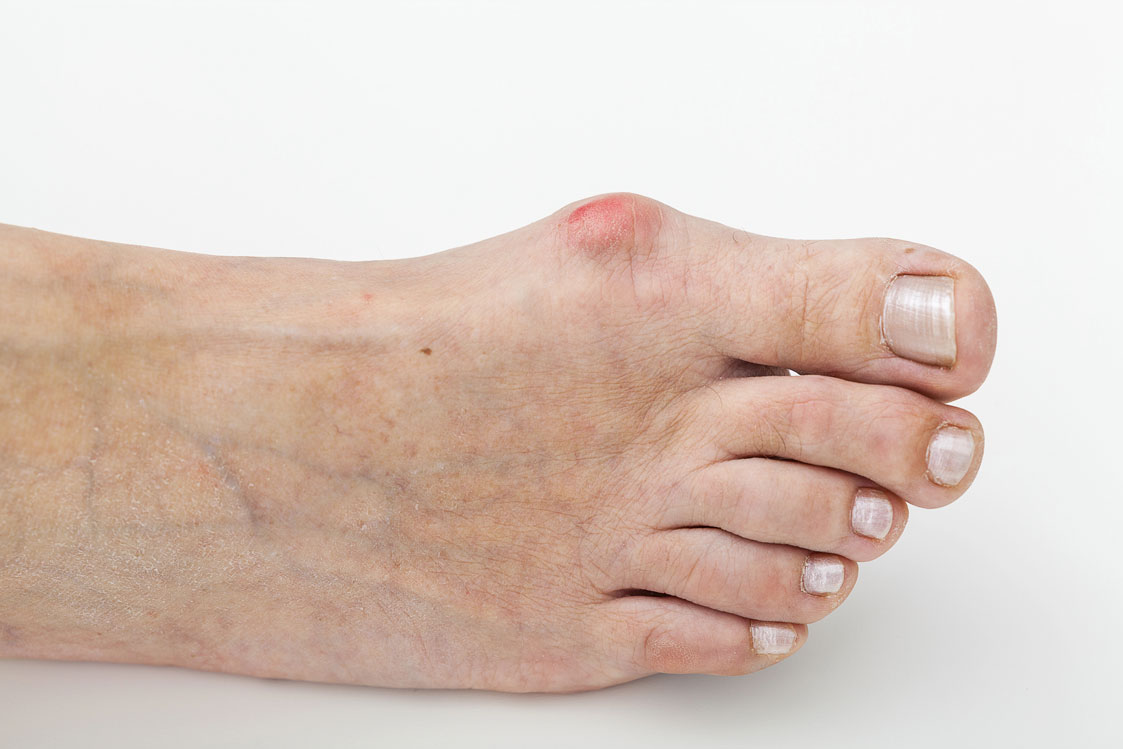
Relief for Your Bunion Pain: A Surgical Solution
Bunions develop due to misalignment of the joint at the base of the big toe. This misalignment can cause the big toe to angle inwards, pushing against the other toes and creating a bony bump on the joint. Minimally invasive bunionectomy procedures address this misalignment, alleviating pain and pressure on the bunion area.
Here’s a closer look at the benefits of minimally invasive bunionectomy surgery:
- Reduced Pain and Discomfort: Surgery can significantly reduce pain and inflammation associated with bunions, allowing you to walk and participate in daily activities without discomfort.
- Improved Appearance: Bunionectomy corrects the misalignment of the big toe, resulting in a more balanced and aesthetically pleasing appearance of your foot.
- Enhanced Mobility: By alleviating pain and pressure, bunionectomy surgery can significantly improve your range of motion in the big toe joint, allowing for more comfortable walking and participation in physical activities.
- Faster Recovery: Minimally invasive techniques typically involve smaller incisions and quicker recovery times than traditional bunionectomy procedures.
Medical Tourism: A Pathway to Affordable Relief
The high cost of bunionectomy surgery in the US can often be a barrier to treatment. Medical tourism offers a compelling alternative, allowing access to high-quality surgery at a fraction of the typical US cost. Imagine waking up pain-free after bunionectomy surgery, followed by a relaxing recovery period in a new destination. Medical tourism lets you seamlessly blend the allure of travel with the expertise of board-certified foot and ankle surgeons abroad, making it a strategic choice for regaining pain-free mobility.
How Much Can I Save?
The significant cost savings offered by medical tourism can be a driving factor for those considering bunionectomy surgery. Here’s a glimpse into the price disparity between the US and popular medical tourism destinations for bunionectomy surgery:
| Country | Estimated Range for Bunionectomy (USD) | Important Note |
|---|---|---|
| United States | $3,500 - $10,000+ | Prices vary depending on the surgeon's experience, location, facility fees, and anesthesia type. |
| Mexico | $1,500 - $3,500 | Consider travel and potential communication barriers. Research facility accreditations and surgeon qualifications. |
| Costa Rica | $2,000 - $4,000 | Similar considerations as Mexico regarding travel and communication. Focus on JCI-accredited facilities and board-certified surgeons. |
| Colombia | $1,200 - $3,000 | It is a popular choice, but thorough research is crucial. Ensure JCI accreditation and surgeon qualifications. |
| Thailand | $800 - $2,000 | It is a budget-friendly option, but significant research is necessary due to varying quality standards. Choose JCI-accredited facilities and board-certified surgeons. |
| India | $700 - $2,500 | The most comprehensive range is due to varying quality standards. Extensive research of facilities, surgeon credentials, and accreditations is essential. |
| Hungary | $1,500 - $3,000 | Offers a balance between affordability and quality care in Europe. Look for JCI accreditation and surgeon qualifications. |
| Poland | $1,200 - $2,800 | Similar considerations as Hungary regarding affordability and quality. Research JCI accreditation and surgeon qualifications. |
| Czech Republic | $1,000 - $2,500 | Similar considerations as Hungary and Poland regarding affordability and quality. Research JCI accreditation and surgeon qualifications. |
| Spain | $1,800 - $3,500 | Popular European destination with high-quality facilities. Research surgeon experience and facility accreditations. |
Please note: These are average costs and can vary depending on the surgeon’s experience, facility fees, the specific procedure (type of bunionectomy), and post-surgical care needs. It’s crucial to get quotes directly from clinics you’re considering.
By carefully considering minimally invasive bunionectomy surgery and exploring medical tourism options, you can take the first step towards a pain-free future and reclaim the joy of movement.
Which Countries Specialize in Bunion Surgery?
The high cost of bunionectomy surgery in the US shouldn’t limit your ability to walk pain-free. Medical tourism offers a compelling solution, granting access to high-quality, minimally invasive bunionectomy procedures at a fraction of the typical US expense. But remember, prioritizing expertise in surgeons and facilities is crucial for a successful outcome.
This article explores popular medical tourism destinations renowned for specializing in minimally invasive bunionectomy surgery:
Central and South America
Costa Rica: Beyond its natural beauty, Costa Rica attracts medical tourists seeking affordable bunionectomy surgery. Costa Rican foot and ankle surgeons are experienced in minimally invasive techniques, promoting a faster return to daily activities. Affordability and proximity to the US make it a convenient option. Ensure JCI accreditation for the facility and surgeon certification from the Costa Rican College of Podiatrists (Colegio de Cirujanos Ortopédicos y Podólogos de Costa Rica).
Mexico: Mexico offers a budget-friendly option for bunionectomy surgery. Many facilities are located near the US border, making travel convenient. However, thorough research is crucial. Look for JCI-accredited facilities and surgeons certified by the Mexican Council of Orthopedics (Consejo Mexicano de Ortopedia).
Asia
India: India has emerged as a leader in medical tourism, offering bunionectomy surgery at a significant cost savings compared to the US. While affordability is a draw, India also boasts a growing pool of highly skilled foot and ankle surgeons experienced in minimally invasive bunionectomy techniques. Remember, thorough research is crucial. Ensure JCI accreditation for the facility and surgeon certification from the Indian Board of Orthopaedics (IBO).
South Korea: A global leader in medical technology, South Korea is also making strides in medical tourism for foot and ankle surgery. South Korean foot and ankle surgeons are known for their advanced techniques and focus on minimally invasive approaches, leading to faster recovery times. Research JCI accreditation for the facility and surgeon certification from the Korean Foot and Ankle Society (KFAS).
Europe
Czech Republic: This European nation is gaining recognition for its foot and ankle surgery expertise, with surgeons experienced in minimally invasive bunionectomy techniques promoting faster recovery times and minimal scarring. Look for JCI-accredited facilities and surgeons certified by the Czech Medical Chamber.
Poland: Similar to the Czech Republic, Poland offers high-quality care at affordable prices. Polish foot and ankle surgeons are well-versed in minimally invasive bunionectomy, ensuring a faster return to daily activities. Verify JCI accreditation for the facility and surgeon certification from the Polish Society of Orthopaedics and Traumatology (PTOiTr).
Spain: A popular European choice for medical tourism, Spain boasts advanced medical facilities and highly skilled foot and ankle surgeons. Spanish surgeons are experienced in various bunionectomy techniques, including minimally invasive approaches for optimal results. Research JCI accreditation for the facility and surgeon certification from the Spanish Society of Foot and Ankle Surgery (SECP).
Remember: While cost savings are a significant factor, prioritizing your health is paramount. Focus on JCI-accredited facilities and surgeons with board certification from your chosen destination’s relevant national foot and ankle surgery association. By carefully researching your options, you can confidently embark on your journey to regaining pain-free movement and enjoying life on your own two feet again.
What Is the Recovery Process?
The ultimate goal after bunionectomy surgery is to walk pain-free and reclaim your active lifestyle. Minimally invasive techniques are becoming increasingly common, but understanding the recovery process is crucial for optimal results. This article explores the typical recovery timeline and provides valuable tips to optimize your journey back to pain-free movement.
Preparing for a Smooth Recovery
Even before your bunionectomy abroad, you can take proactive steps to ensure a smooth recovery:
- Pre-Operative Conditioning: Strengthen your foot and ankle muscles through exercises prescribed by your doctor or physical therapist. Stronger muscles will aid in a faster and more complete recovery after surgery.
- Post-Surgical Care Options: Discuss post-surgical care with your doctor. Some hospitals or clinics may offer rehabilitation packages tailored to bunionectomy recovery. Explore these options and inquire about the qualifications of the physical therapists involved.
- Packing Essentials: Pack comfortable shoes with good arch support to accommodate post-surgical swelling. Consider bringing a compression stocking to help manage swelling and a supportive brace for added stability, especially if recommended by your doctor.
The Bunionectomy Recovery Timeline
- Hospital Stay: Following successful surgery, you can expect a short hospital stay, typically less than 24 hours, depending on the complexity of the procedure and the facility’s protocols.
- Physical Therapy: Physical therapy may begin as early as the day after surgery and continue for several weeks in the hospital or as an outpatient. These exercises focus on regaining strength, flexibility, and range of motion in your ankle and foot.
- Pain Management: Your doctor will prescribe pain medication to manage post-surgical discomfort. It’s essential to follow their instructions carefully and taper off medicines as directed.
- Returning Home: Depending on your progress and comfort level, you can return home within a day, often with specific instructions for ongoing physical therapy and home care.
Recovery at Home: Essential Steps for Success
Following discharge, continued recovery at home is crucial:
- Physical Therapy: Regular physical therapy exercises are essential for regaining foot and ankle mobility and function. These exercises can be performed at home or in an outpatient physical therapy clinic, depending on your progress and the complexity of the surgery.
- Rest and Activity Balance: While rest is necessary for healing, gentle movement is crucial to prevent stiffness. As your body tolerates them, ankle and foot stretches, as well as light activities like walking short distances, are encouraged.
- Precautions: To prevent complications, avoiding strenuous activities that could strain your foot or ankle is essential. This may include heavy lifting, prolonged standing, or high-impact activities until your doctor clears you.
- Pain Management: Continue taking pain medication as your doctor prescribes, gradually reducing it as your pain improves.
- Scar Management: If you have any scarring, your doctor may recommend scar massage techniques or silicone scar sheets to minimize their appearance.
Additional Considerations for a Successful Recovery
- Communication: Ensure clear communication with your doctor throughout the process, before and after you return home. Don’t hesitate to ask questions or voice concerns, especially if you’re recovering from surgery abroad.
- Follow-Up Care: Schedule appointments with your doctor or surgeon to monitor your progress and ensure proper healing. This may involve follow-up consultations in your home country or virtually with a doctor abroad.
Remember: Recovery from bunionectomy surgery is a gradual process. Be patient with yourself, listen to your body, and focus on following your doctor’s instructions and physical therapy routines. By following these guidelines and adhering to your recovery plan, you’ll be well on your way to enjoying pain-free movement and returning to the activities you love.
What Are Some Risks And Complications?
Bunionectomy surgery, while minimally invasive and highly effective in relieving bunion pain, carries potential risks and complications like any surgical procedure. Understanding these possible issues can empower you to make informed decisions about your bunion treatment plan.
Common Complications
Bleeding and Infection: While uncommon, bleeding and infection are possible risks after bunionectomy surgery. Bleeding can occur during or after surgery, and infection can develop if sterile techniques aren’t strictly followed. Choosing a board-certified foot and ankle surgeon and diligently following post-operative instructions can minimize these risks. Open communication with your doctor throughout the process is essential.
Swelling and Bruising: Swelling and bruising around the foot and incision site are joint after bunionectomy surgery. The extent and duration of swelling will vary depending on the individual, but it typically subsides gradually over several weeks. Pain medication can help manage discomfort during this initial healing phase.
Scarring: Scarring is inevitable with any surgery, and bunionectomy is no exception. However, skilled foot and ankle surgeons aim for minimal incisions and utilize techniques that minimize scar visibility. A proper scar care regimen is crucial for optimal healing and reducing scar prominence. Your surgeon might recommend silicone gel sheets or scar massage therapy.
Pain and Discomfort: Some discomfort and pain are expected after surgery, and your surgeon will prescribe medication to manage them effectively. The discomfort usually eases within the first few days or weeks as healing progresses.
Stiffness: Stiffness in the ankle and foot can occur after surgery, limiting your range of motion. Physical therapy is often recommended to regain flexibility and movement.
Uncommon Complications
Nerve Injury: Although nerve damage during surgery is uncommon, it can lead to weakness, numbness, or tingling in the toes or foot.
Remember: Communication with your board-certified foot and ankle surgeon is vital. Discuss your expectations, potential risks of bunionectomy surgery, and any concerns. Choosing a qualified surgeon with experience in bunionectomy significantly reduces the risk of complications and helps ensure a successful outcome.
Am I a Good Candidate for Bunion Surgery?
Bunion pain can significantly impact your mobility and quality of life. While minimally invasive bunionectomy surgery offers a lasting solution, it’s only for some. This self-assessment guide can help you determine if bunionectomy might be the right course of action for you.
Severity of Symptoms
Do you experience persistent pain, swelling, redness, or stiffness at the base of your big toe? Has the bunion deformity progressively worsened, causing your big toe to crowd or overlap your other toes? Are these symptoms interfering with your ability to walk comfortably or wear shoes that fit properly?
Failure of Conservative Treatments
Do conservative treatments like orthopedic inserts, wider shoes, toe spacers, icing, anti-inflammatory medications, or activity modification not adequately relieve your bunion pain?
Impact on Daily Life
Does bunion pain significantly limit your ability to participate in activities you enjoy, such as walking, running, or exercising? Does it restrict your choice of footwear or make it difficult to stand or walk for extended periods?
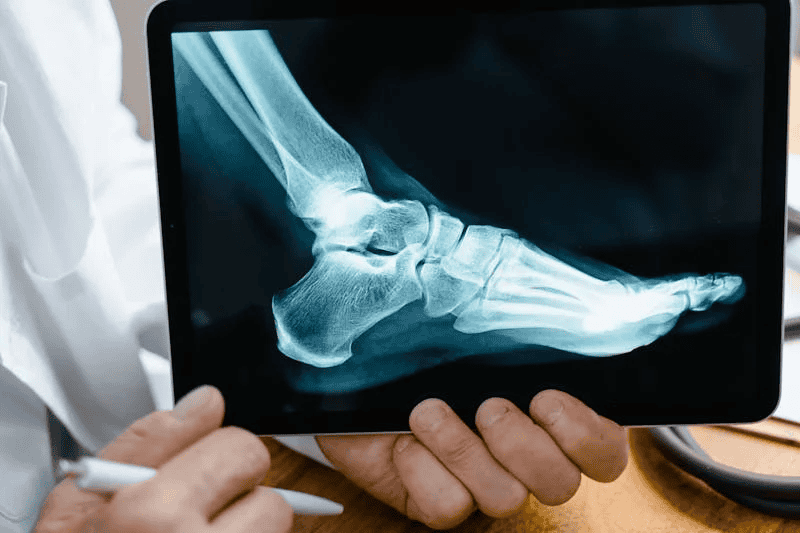
Seeking Professional Guidance
This self-assessment can be a helpful starting point, but consulting a board-certified foot and ankle surgeon is crucial for a definitive answer. Here’s what to expect during your consultation:
- Medical History Review: Your doctor will review your medical history, including any pre-existing conditions and medications you take.
- Physical Examination: A thorough physical examination will assess your foot and ankle for bunion deformity, joint mobility, and signs of inflammation.
- Imaging Tests: X-rays or other imaging tests may be recommended to evaluate the severity of the bunion and assess your bone structure.
- Discussion of Treatment Options: Your doctor will discuss the potential benefits and risks of bunionectomy surgery compared to other treatment options, such as physical therapy or bracing.
Additional Considerations
- Recovery Timeline: Recovery time varies depending on the surgical approach and the severity of your bunion. Following surgery, physical therapy may be recommended to regain strength and flexibility in your foot and ankle.
- Long-Term Management: While bunionectomy surgery can provide significant pain relief and improve alignment, proper footwear choices, and activity modifications might still be necessary to prevent recurrence.
Remember: Open communication with your doctor throughout the process is essential. Discuss your concerns about bunionectomy surgery and ensure you understand the potential benefits and risks. By carefully considering these factors and consulting with a qualified healthcare professional, you can determine if bunionectomy surgery is the right path to restore pain-free movement and get you back on your feet comfortably.
What is Bunion Surgery (Bunionectomy)?
Bunion pain can significantly disrupt your mobility and daily routine. Bunionectomy surgery offers a lasting solution, but understanding the procedure is essential for making informed decisions. This article delves into bunionectomy surgery, explaining what it entails and the benefits it can offer.
What is a Bunion?
A bunion is a bony bump that forms at the base of your big toe, where the joint connects to your metatarsal bone (the long bone in your foot). The big toe may angle inwards towards the other toes, causing them to crowd or overlap. This deformity can develop due to various factors, including genetics, improper footwear, and specific foot conditions.
What is Bunionectomy Surgery?
Bunionectomy surgery is a minimally invasive procedure designed to correct the bunion deformity and realign your big toe. There are different surgical techniques, but all aim to achieve the same goal: alleviate pain and improve foot function. Here’s a simplified overview of the typical procedure:
Following carpal tunnel release surgery, you can expect:
- Anesthesia: Bunionectomy surgery is typically performed on an outpatient basis under local anesthesia with sedation. In some cases, general anesthesia might be used.
- Incision: The surgeon makes a small incision on the top or side of your foot near the bunion.
Bone Realignment: The surgeon removes or repositions a portion of the bone involved in the bunion formation. This realigns the big toe into a more natural position. - Soft Tissue Repair: To improve flexibility and alignment, any tightened tendons or ligaments around the joint might be adjusted or released.
- Closure: The incision is then closed with stitches or surgical glue.
Benefits of Bunionectomy Surgery
Bunionectomy surgery offers significant benefits for individuals experiencing pain and limitations due to bunions. Here are some key advantages:
- Pain Relief: The primary benefit is eliminating pain and discomfort at the bunion site. This allows for pain-free walking, standing, and participation in various activities.
- Improved Alignment: By correcting the big toe’s angulation, bunionectomy surgery restores proper foot alignment and biomechanics. This reduces pressure on the joint and surrounding tissues, preventing further pain and discomfort.
- Enhanced Mobility: Bunionectomy surgery can significantly enhance mobility by reducing pain and improving alignment. Activities like walking, running, and exercise become more manageable and enjoyable.
- Better Shoe Fit: The corrected toe position allows you to wear shoes that fit comfortably and provide proper support. This can significantly improve your overall comfort and quality of life.
Considering Bunionectomy Surgery?
Consulting a board-certified foot and ankle surgeon is crucial if you’re experiencing persistent bunion pain and limitations in your daily activities. They can discuss your situation, assess your bunion’s severity, and determine if bunionectomy surgery is the right course of action for you. Early diagnosis and treatment can significantly improve your foot health and overall well-being.
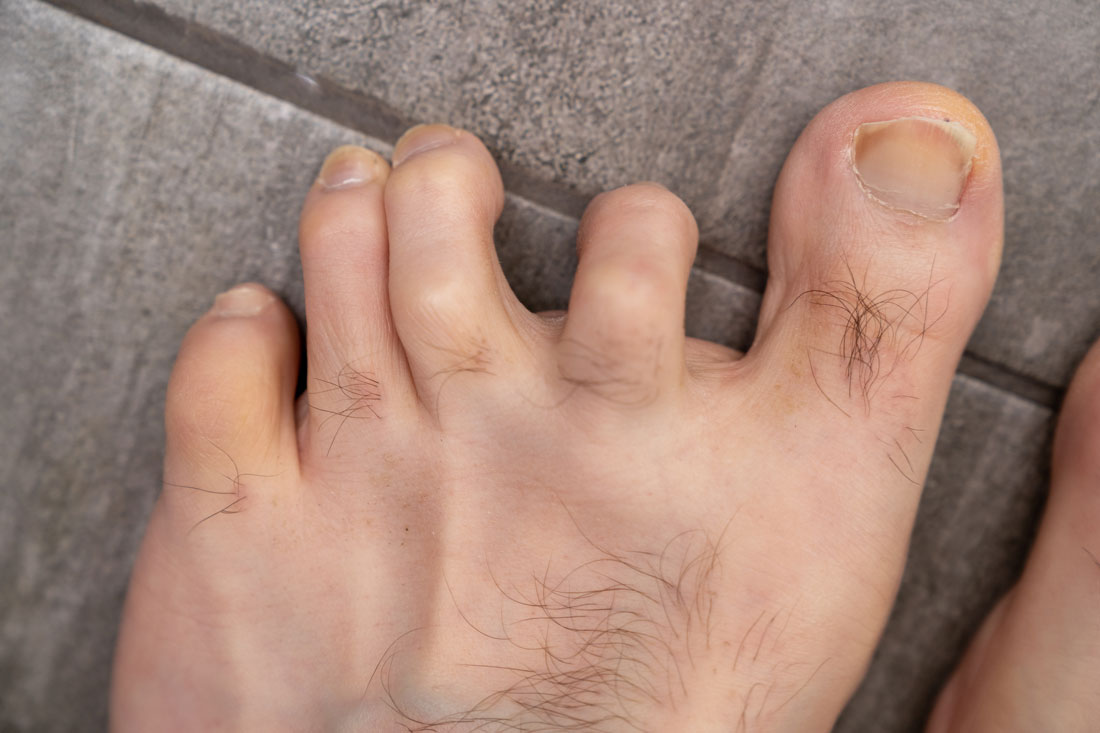
Hammertoes
Our feet, the tireless workhorses that carry us throughout our lives, deserve proper care. But, a common condition called hammertoes can disrupt this balance, causing discomfort and limiting mobility. Hammertoes occur when the middle joint of one or more toes bends downwards, resembling a curled claw. This deformity can develop due to various factors, including ill-fitting shoes, certain foot conditions, or genetics.
The high cost of hammertoe correction surgery in the US can often be a barrier to treatment. Thankfully, medical tourism offers a compelling alternative, allowing access to high-quality surgery at a fraction of the typical US cost. Imagine waking up pain-free after hammertoe correction surgery, followed by a relaxing recovery period in a new destination. Medical tourism lets you seamlessly blend the allure of travel with the expertise of board-certified podiatrists or foot and ankle surgeons abroad, making it a strategic choice for regaining pain-free mobility.
How Much Can I Save?
While the exact cost can vary depending on factors like surgeon experience, facility fees, and the specific procedure needed, this table provides a general comparison of the expenses between the US and popular medical tourism destinations:
| Country | Estimated Range for Hammertoe Correction Surgery (USD) | Important Note |
|---|---|---|
| United States | $3,000 - $7,000+ | Prices vary depending on the surgeon's experience, location, facility fees, and anesthesia type. |
| Mexico | $1,200 - $3,000 | Consider travel and potential communication barriers. Research facility accreditations and surgeon qualifications (board certification). |
| Costa Rica | $1,500 - $3,500 | Similar considerations as Mexico regarding travel and communication. Focus on JCI-accredited facilities and board-certified surgeons. |
| Colombia | $1,000 - $2,500 | It is a popular choice, but thorough research is crucial. Ensure JCI accreditation and surgeon qualifications (board certification). |
| Thailand | $800 - $2,000 | It is a budget-friendly option, but significant research is necessary due to varying quality standards. Choose JCI-accredited facilities and board-certified surgeons. |
| India | $600 - $2,000 | The most comprehensive range is due to varying quality standards. Extensive research of facilities, surgeon credentials, and accreditations (board certification) is essential. |
| Hungary | $1,200 - $2,800 | Offers a balance between affordability and quality care in Europe. Look for JCI accreditation and surgeon qualifications (board certification). |
| Poland | $1,000 - $2,500 | Similar considerations as Hungary regarding affordability and quality. Research JCI accreditation and surgeon qualifications (board certification). |
| Czech Republic | $800 - $2,000 | Similar considerations as Hungary and Poland regarding affordability and quality. Research JCI accreditation and surgeon qualifications (board certification). |
| Spain | $1,500 - $3,000 | Popular European destination with high-quality facilities. Research surgeon experience and facility accreditations. |
Important Note
- These are average costs and can vary depending on the surgeon’s experience, facility fees, the specific procedure (type of hammertoe correction), and post-surgical care needs. It’s crucial to get quotes directly from clinics you’re considering.
- JCI accreditation signifies that a medical facility meets rigorous international standards for quality care.
- Board certification ensures your surgeon has the qualifications and experience to perform hammertoe correction surgery.
By carefully considering minimally invasive hammertoe correction surgery and exploring medical tourism options, you can take the first step towards a pain-free future and reclaim the joy of movement without breaking the bank.
Which Countries Specialize in Hammertoe Correction Surgery?
Hammertoes can significantly disrupt your active lifestyle, causing pain and limiting mobility. The high cost of minimally invasive hammertoe correction surgery in the US can be a discouraging barrier to treatment. Thankfully, medical tourism offers a solution, granting access to high-quality procedures at a fraction of the typical US expense. However, prioritizing surgeon expertise and facility quality is crucial for a successful outcome.
Central and South America
- Costa Rica: Beyond its stunning rainforests, Costa Rica attracts medical tourists seeking affordable hammertoe correction surgery. Costa Rican foot and ankle surgeons are experienced in minimally invasive techniques, promoting a faster return to daily activities. Affordability and proximity to the US make it a convenient option. Ensure JCI accreditation for the facility and surgeon certification from the Costa Rican College of Podiatrists (Colegio de Cirujanos Ortopédicos y Podólogos de Costa Rica).
- Colombia: Emerging as a leader in medical tourism, Colombia offers hammertoe correction surgery at significant cost savings compared to the US. Colombian foot and ankle surgeons are increasingly skilled in minimally invasive techniques. Remember, thorough research is crucial. Look for JCI-accredited facilities and surgeons certified by the Colombian Society of Orthopaedics and Traumatology (Sociedad Colombiana de Ortopedia y Traumatología – SCOT).
Europe
- Czech Republic: This European nation is gaining recognition for its foot and ankle surgery expertise. Surgeons experienced in minimally invasive hammertoe correction techniques promote faster recovery times and minimal scarring. Look for JCI-accredited facilities and surgeons certified by the Czech Medical Chamber.
- Poland: Similar to the Czech Republic, Poland offers high-quality care at affordable prices. Polish foot and ankle surgeons are well-versed in minimally invasive hammertoe correction, ensuring a faster return to daily activities. Verify JCI accreditation for the facility and surgeon certification from the Polish Society of Orthopaedics and Traumatology (PTOiTr).
- Hungary: Hungary offers a balance between affordability and quality care in Europe. Hungarian foot and ankle surgeons are increasingly experienced in minimally invasive hammertoe correction procedures. Look for JCI-accredited facilities and surgeons certified by the Hungarian Society of Orthopaedics (Magyar Ortopédiai Társaság – MOT).
- India: India remains a leader in medical tourism, offering hammertoe correction surgery at a significant cost savings compared to the US. While affordability is a draw, India also boasts a growing pool of highly skilled foot and ankle surgeons experienced in minimally invasive techniques. Remember, thorough research is crucial. Ensure JCI accreditation for the facility and surgeon certification from the Indian Board of Orthopaedics (IBO).
- Thailand: A budget-friendly option for medical tourism, Thailand offers hammertoe correction surgery at attractive prices. However, extensive research is necessary due to varying quality standards. Choose JCI-accredited facilities and surgeons certified by the Thai Medical Council and the Thai Orthopaedic Association.
Remember: While cost savings are a significant factor, prioritizing your health is paramount. Focus on JCI-accredited facilities and surgeons with board certification from your chosen destination’s relevant national foot and ankle surgery association. By carefully researching your options, you can confidently embark on your journey to pain-free toes and reclaim your active lifestyle.
What Is the Recovery Process for Hammertoe Correction Surgery?
Minimally invasive hammertoe correction surgery offers a solution to reclaim pain-free movement in your toes. However, understanding the recovery process is crucial for optimal results, especially if you’re considering medical tourism. This article explores the typical recovery timeline for hammertoe correction surgery and provides valuable tips to optimize your journey back to pain-free mobility.
Preparing for a Smooth Recovery
Even before your hammertoe correction surgery abroad, you can take proactive steps to ensure a smooth recovery:
- Pre-Operative Conditioning: Strengthen your foot and ankle muscles through exercises prescribed by your doctor or physical therapist. Stronger muscles will aid in a faster and more complete recovery after surgery.
- Post-Surgical Care Options: Discuss post-surgical care with your doctor. Some hospitals or clinics may offer rehabilitation packages tailored to hammertoe correction recovery. Explore these options and inquire about the qualifications of the physical therapists involved.
- Packing Essentials: Pack comfortable, wide-toed shoes with good arch support to accommodate post-surgical swelling. Consider bringing a compression stocking to help manage swelling and a supportive bandage or brace for added stability, especially if recommended by your doctor.
The Hand and Wrist Tendon Repair Recovery Timeline
- Hospital Stay: Following successful surgery, you can expect a short hospital stay, typically less than 24 hours, depending on the complexity of the procedure and the facility’s protocols.
- Physical Therapy:Physical therapy may begin as early as the day after surgery and continue for several weeks in the hospital or as an outpatient. These exercises focus on regaining strength, flexibility, and range of motion in your wrist and hand.
- Pain Management: Your doctor will prescribe pain medication to manage post-surgical discomfort. It’s crucial to follow their instructions carefully and taper off medications as directed.
- Returning Home: Depending on your progress and comfort level, you can return home within a day, often with specific instructions for ongoing physical therapy and home care.
The Hammertoe Correction Recovery Timeline
- Hospital Stay: Following successful surgery, you can expect a short hospital stay, typically less than 24 hours, depending on the complexity of the procedure and the facility’s protocols.
- Physical Therapy: Physical therapy may begin as early as the day after surgery and continue for several weeks in the hospital or as an outpatient. These exercises focus on regaining strength, flexibility, and range of motion in your toes, ankle, and foot.
- Pain Management: Your doctor will prescribe pain medication to manage post-surgical discomfort. It’s essential to follow their instructions carefully and taper off medicines as directed.
- Returning Home: Depending on your progress and comfort level, you can return home within a day, often with specific instructions for ongoing physical therapy and home care.

Recovery at Home: Essential Steps for Success
Following discharge, continued recovery at home is crucial:
- Physical Therapy: Regular physical therapy exercises are essential for regaining mobility and function in the toe, ankle, and foot. These exercises can be performed at home or in an outpatient physical therapy clinic, depending on your progress and the complexity of the surgery.
- Rest and Activity Balance: While rest is necessary for healing, gentle movement is crucial to prevent stiffness. As your body tolerates them, ankle and foot stretches, as well as light activities like walking short distances, are encouraged.
- Precautions: To prevent complications, avoiding strenuous activities that could strain your foot or toes is essential. This may include heavy lifting, prolonged standing, or high-impact activities until your doctor clears you.
- Pain Management: Continue taking pain medication as your doctor prescribes, gradually reducing it as your pain improves.
- Scar Management: If you have any scarring, your doctor may recommend scar massage techniques or silicone scar sheets to minimize their appearance.
Additional Considerations for a Successful Recovery
- Communication: Ensure clear communication with your doctor throughout the process, before and after you return home. Don’t hesitate to ask questions or voice concerns, especially if you’re recovering from surgery abroad.
- Follow-Up Care: Schedule appointments with your doctor or surgeon to monitor your progress and ensure proper healing. This may involve follow-up consultations in your home country or virtually with a doctor abroad.
Remember: Recovery from hammertoe correction surgery is a gradual process. Be patient with yourself, listen to your body, and focus on following your doctor’s instructions and physical therapy routines. By following these guidelines and adhering to your recovery plan, you’ll be well on your way to enjoying pain-free toes and returning to the activities you love.
What Are Some Risks and Complications of Hammertoe Correction Surgery?
Minimally invasive hammertoe correction surgery offers a path to pain-free toes, but like any surgery, it carries potential risks and complications. Understanding these potential issues empowers you to make informed decisions about your hammertoe treatment plan.
Common Complications
Bleeding and Infection: While uncommon, bleeding and infection are possible risks after hammertoe correction surgery. Bleeding can occur during or after surgery, and infection can develop if sterile techniques aren’t strictly followed. Choosing a board-certified podiatrist or foot and ankle surgeon and diligently following post-operative instructions can minimize these risks. Open communication with your doctor throughout the process is essential.
Swelling and Bruising: After hammertoe correction surgery, swelling and bruising around the toes and incision site are common. The extent and duration of swelling will vary depending on the individual, but it typically subsides gradually over several weeks. Pain medication can help manage discomfort during this initial healing phase.
Scarring: Scarring is inevitable with any surgery, and hammertoe correction is no exception. However, skilled podiatrists or foot and ankle surgeons aim for minimal incisions and utilize techniques that minimize scar visibility. A proper scar care regimen is crucial for optimal healing and reducing scar prominence. Your surgeon might recommend silicone gel sheets or scar massage therapy.
Pain and Discomfort: Some discomfort and pain are expected after surgery, and your surgeon will prescribe medication to manage them effectively. The discomfort usually eases within the first few days or weeks as healing progresses.
Stiffness: After surgery, stiffness in the toes, ankle, and foot can occur, limiting your range of motion. Physical therapy is often recommended to regain flexibility and movement.
Uncommon Complications
Nerve Injury: Although nerve damage during surgery is uncommon, it can lead to weakness, numbness, or tingling in the toes or foot.
Incomplete Hammertoe Correction: In rare cases, the hammertoe deformity might not be entirely corrected during surgery. Revision surgery might be necessary to address this issue.
Complex Regional Pain Syndrome (CRPS): This rare condition, formerly known as Reflex Sympathetic Dystrophy (RSD), is characterized by chronic pain, swelling, and stiffness that can develop after surgery. There is no known cause, and treatment can be challenging.
Remember: Communication with your board-certified podiatrist or foot and ankle surgeon is vital. Discuss your expectations, potential risks of hammertoe correction surgery, and any concerns. Choosing a qualified surgeon with experience in hammertoe correction significantly reduces the risk of complications and helps ensure a successful outcome.
Am I a Good Candidate for Hammertoe Correction Surgery?
Hammertoes can significantly disrupt your active lifestyle, causing pain and limiting mobility. Minimally invasive hammertoe correction surgery offers a solution, but only for some. This self-assessment guide can help you determine if hammertoe correction surgery might be the right course of action for you.
Severity of Symptoms
- Pain: Do you experience persistent pain at the tip or joint of your affected toes? Does the pain worsen with activity, such as walking or standing for extended periods?
- Deformity: Have your toes become bent downwards, resembling a claw? Has the deformity progressively worsened over time?
- Limited Mobility: Do hammertoes restrict the natural movement of your toes, affecting your balance or gait?
- Difficulties with Footwear: Do you have trouble finding shoes that accommodate bent toes, causing further discomfort?
Failure of Conservative Treatments
- Non-surgical options: Have conservative treatments like orthotics, wider shoes, toe spacers, icing, pain medication, or activity modification not provided adequate relief?
Impact on Daily Life
- Activity limitations: Does hammertoe pain significantly limit your ability to participate in activities you enjoy, such as walking, running, or exercising?
- Footwear choices: Do hammertoes restrict your choice of footwear or make it difficult to stand or walk for extended periods?
Seeking Professional Guidance
This self-assessment can be a helpful starting point, but consulting a board-certified podiatrist or foot and ankle surgeon is crucial for a definitive answer. Here’s what to expect during your consultation:
- Medical History Review: Your doctor will review your medical history, including any pre-existing conditions and medications you take.
- Physical Examination: A thorough physical examination will assess your toes, foot, and ankle for hammertoe deformity, joint mobility, and signs of inflammation.
- Imaging Tests: X-rays or other imaging tests may be recommended to evaluate the severity of the hammertoes and assess your bone structure.
- Treatment Options Discussion: Your doctor will discuss hammertoe correction surgery’s potential benefits and risks compared to other options, such as physical therapy or splinting.
Additional Considerations
- Recovery Timeline: Recovery time varies depending on the surgical approach and the severity of your hammertoes. Following surgery, physical therapy may be recommended to regain strength and flexibility in your toes, foot, and ankle.
- Long-Term Management: While hammertoe correction surgery can provide significant pain relief and improve toe alignment, proper footwear choices, and activity modifications might still be necessary to prevent a recurrence.
Remember: Open communication with your doctor throughout the process is essential. Discuss your concerns about hammertoe correction surgery and ensure you understand the potential benefits and risks. By carefully considering these factors and consulting with a qualified healthcare professional, you can determine if hammertoe correction surgery is the right path to walk comfortably and pain-free again.
What Is Hammertoe Correction Surgery?
Hammertoes can significantly disrupt an active lifestyle, causing pain and limiting mobility. Hammertoe correction surgery offers a solution, but what exactly does it entail? This article explores the procedure, explaining its purpose and the benefits it can provide.
What is a Hammertoe?
A hammertoe is a deformity where one or more toes bend downward at the middle joint, resembling a claw. This can occur due to various factors, including:
- Genetics: Inherited foot structure can predispose you to hammertoes.
- Improper footwear: Too tight or pointed shoes can crowd toes and contribute to deformity.
- Muscle imbalances: Weak or imbalanced muscles in the foot can lead to hammertoe development.
- Arthritis: Degenerative joint disease can affect the toe joints, causing them to bend abnormally.
What is Hammertoe Correction Surgery?
Hammertoe correction surgery is a minimally invasive procedure designed to straighten the affected toe and restore proper alignment. There are different surgical techniques, but all aim to alleviate pain and improve toe function. Here’s a simplified overview of the typical procedure:
- Anesthesia: Hammertoe correction surgery is typically performed by outpatients under local anesthesia with sedation. In some cases, general anesthesia might be used.
- Incision: Depending on the location and severity of the hammertoe, the surgeon makes a small incision on the top or side of the toe.
- Bone Correction: Depending on the severity of the deformity, the surgeon may need to remove a small portion of the bone or realign the existing bone to straighten the toe joint.
- Soft Tissue Adjustments: Tightened tendons or ligaments around the joint might be released or repaired to improve flexibility and alignment.
- Immobilization: In some cases, a splint or bandage might be applied to the toe to stabilize it and promote proper healing.
- Closure: The incision is then closed with stitches or surgical glue.
Benefits of Hammertoe Correction Surgery
Hammertoe correction surgery significantly benefits individuals experiencing pain and limitations due to hammertoes. Here are some key advantages:
- Pain Relief: The primary benefit is eliminating pain and discomfort at the affected toe joint. This allows for pain-free walking, standing, and participation in various activities.
- Improved Alignment: Hammertoe correction surgery restores proper toe alignment by straightening the bent toe. This reduces pressure on the joint and surrounding tissues, preventing further pain and discomfort.
- Enhanced Mobility: Alleviating pain and improving toe alignment can significantly enhance mobility. Activities like walking, running, and exercise become more manageable and enjoyable.
- Better Shoe Fit: The corrected toe position allows you to wear shoes that fit comfortably and provide proper support. This can significantly improve your overall comfort and quality of life.
- Prevention of Further Complications: Hammertoes can worsen over time, leading to additional problems like corns, calluses, and open wounds. Early correction can prevent these complications.
Considering Hammertoe Correction Surgery?
Consulting a board-certified podiatrist or foot and ankle surgeon is crucial if you’re experiencing persistent hammertoe pain and limitations in your daily activities. They can discuss your situation, assess the severity of your hammertoes, and determine if hammertoe correction surgery is the right course of action for you. Early diagnosis and treatment can significantly improve your foot health and overall well-being.
Plantar Fasciitis Surgery
Our feet, the tireless workhorses that carry us throughout life, deserve the utmost care. Plantar fasciitis, a condition causing sharp heel pain, can significantly disrupt your mobility and daily activities. For many Americans, the high cost of plantar fasciitis surgery can be a barrier to seeking a permanent solution. Thankfully, minimally invasive surgical procedures offer long-lasting relief, and medical tourism unlocks access to high-quality care at a fraction of the typical US expense.
Imagine waking up pain-free after plantar fasciitis surgery, followed by a relaxing recovery period in a new destination. Medical tourism allows you to seamlessly blend the allure of travel with the expertise of board-certified podiatrists or foot and ankle surgeons abroad, making it a strategic choice for regaining a pain-free stride.
How Much Can I Save?
The significant cost savings offered by medical tourism can be a driving factor for those considering plantar fasciitis surgery. Here’s a glimpse into the price disparity between the US and popular medical tourism destinations for plantar fasciitis surgery:
| Country | Estimated Range for Plantar Fasciitis Surgery (USD) | Important Note |
|---|---|---|
| United States | $5,000 - $10,000+ | Prices vary depending on the surgeon's experience, location, facility fees, and anesthesia type. |
| Mexico | $2,000 - $4,000 | Consider travel and potential communication barriers. Research facility accreditations and surgeon qualifications. |
| Costa Rica | $2,500 - $4,500 | Similar considerations as Mexico regarding travel and communication. Focus on JCI-accredited facilities and board-certified surgeons. |
| Colombia | $1,800 - $3,500 | It is a popular choice, but thorough research is crucial. Ensure JCI accreditation and surgeon qualifications. |
| Thailand | $1,200 - $2,500 | It is a budget-friendly option, but significant research is necessary due to varying quality standards. Choose JCI-accredited facilities and board-certified surgeons. |
| India | $1,000 - $3,000 | The most comprehensive range is due to varying quality standards. Extensive research of facilities, surgeon credentials, and accreditations is essential. |
| Hungary | $2,000 - $4,000 | Offers a balance between affordability and quality care in Europe. Look for JCI accreditation and surgeon qualifications. |
| Poland | $1,800 - $3,200 | Similar considerations as Hungary regarding affordability and quality. Research JCI accreditation and surgeon qualifications. |
| Czech Republic | $1,500 - $3,000 | Similar considerations as Hungary and Poland regarding affordability and quality. Research JCI accreditation and surgeon qualifications. |
| Spain | $2,500 - $4,000 | Popular European destination with high-quality facilities. Research surgeon experience and facility accreditations. |
Please note: These are average costs and can vary depending on the surgeon’s experience, facility fees, the specific procedure (type of plantar fasciitis surgery), and post-surgical care needs. It’s crucial to get quotes directly from clinics you’re considering.
By exploring minimally invasive plantar fasciitis surgery and medical tourism options, you can take the first step towards a pain-free future and reclaim the joy of movement without breaking the bank.
Which Countries Specialize in Plantar Fasciitis Surgery?
Plantar fasciitis, a common cause of heel pain, can significantly disrupt mobility and quality of life. In the US, the high cost of minimally invasive plantar fasciitis surgery can be a significant obstacle to seeking treatment. Thankfully, medical tourism offers a compelling solution – access to high-quality surgical procedures at a fraction of the typical US expense. However, prioritizing surgeon expertise and facility quality is crucial for successful outcomes.
Central and South America
- Costa Rica: Beyond its breathtaking natural beauty, Costa Rica attracts medical tourists seeking affordable plantar fasciitis surgery. Costa Rican podiatrists and foot and ankle surgeons are experienced in minimally invasive techniques, promoting a quicker recovery and faster return to daily activities. Affordability and proximity to the US make it a convenient option. Ensure Joint Commission International (JCI) accreditation for the facility and surgeon certification from the Costa Rican College of Podiatrists (Colegio de Cirujanos Ortopédicos y Podólogos de Costa Rica).
- Colombia: Emerging as a leader in medical tourism, Colombia offers plantar fasciitis surgery at significant cost savings compared to the US. Colombian foot and ankle surgeons are increasingly skilled in minimally invasive techniques. Remember, thorough research is crucial. Look for JCI-accredited facilities and surgeons certified by the Colombian Society of Orthopaedics and Traumatology (Sociedad Colombiana de Ortopedia y Traumatología – SCOT).
Europe
- Czech Republic: This European nation is gaining recognition for its foot and ankle surgery expertise. Surgeons experienced in minimally invasive plantar fasciitis procedures promote faster recovery times and minimal scarring. Look for JCI-accredited facilities and surgeons certified by the Czech Medical Chamber.
- Poland: Similar to the Czech Republic, Poland offers high-quality care at affordable prices. Polish podiatrists and foot and ankle surgeons are well-versed in minimally invasive plantar fasciitis correction, ensuring a faster return to a pain-free life. Verify JCI accreditation for the facility and surgeon certification from the Polish Society of Orthopaedics and Traumatology (PTOiTr).
- Hungary: Hungary offers a balance between affordability and quality care in Europe. Hungarian foot and ankle surgeons are increasingly experienced in minimally invasive plantar fasciitis surgery. Look for JCI-accredited facilities and surgeons certified by the Hungarian Society of Orthopaedics (Magyar Ortopédiai Társaság – MOT).
Asia
- India: India remains a leader in medical tourism, offering plantar fasciitis surgery at a significant cost savings compared to the US. While affordability is a draw, India boasts a growing pool of highly skilled podiatrists and foot and ankle surgeons experienced in minimally invasive techniques. Remember, thorough research is crucial. Ensure JCI accreditation for the facility and surgeon certification from the Indian Board of Orthopaedics (IBO).
- Thailand: A budget-friendly option for medical tourism, Thailand offers plantar fasciitis surgery at attractive prices. However, extensive research is necessary due to varying quality standards. Choose JCI-accredited facilities and surgeons certified by the Thai Medical Council and the Thai Orthopaedic Association.
Remember: While cost savings are a significant factor, prioritizing your health is paramount. Focus on JCI-accredited facilities and surgeons with board certification from your chosen destination’s relevant national foot and ankle surgery association. By carefully researching your options, you can confidently embark on your journey to pain-free feet and reclaim an active lifestyle.
What Is the Recovery Process for Plantar Fasciitis Surgery?
Minimally invasive plantar fasciitis surgery offers a permanent solution to heel pain, but understanding the recovery process is crucial, especially if you’re considering medical tourism. This article explores the typical recovery timeline for plantar fasciitis surgery abroad and provides valuable tips to optimize your journey back to pain-free mobility.
Preparing for a Smooth Recovery
Even before your plantar fasciitis surgery abroad, proactive steps can ensure a smooth recovery:
- Pre-Operative Conditioning: Strengthen your calf and foot muscles through exercises prescribed by your doctor or physical therapist. Stronger muscles will aid in a faster and more complete recovery after surgery.
- Post-Surgical Care Options: Discuss post-surgical care with your doctor. Some hospitals or clinics may offer rehabilitation packages tailored to plantar fasciitis recovery. Explore these options and inquire about the qualifications of the physical therapists involved.
- Packing Essentials: Pack comfortable, supportive shoes with good arch support to accommodate post-surgical swelling. Consider bringing a compression stocking to help manage swelling and a supportive bandage or brace for added stability, especially if recommended by your doctor.
The Plantar Fasciitis Surgery Recovery Timeline
- Hospital Stay: Following successful surgery, you can expect a short hospital stay, typically less than 24 hours, depending on the complexity of the procedure and the facility’s protocols.
- Physical Therapy: Physical therapy may begin as early as the day after surgery and continue for several weeks in the hospital or as an outpatient. These exercises improve flexibility and reduce stiffness in your plantar fascia and calf muscles.
- Pain Management: Your doctor will prescribe pain medication to manage post-surgical discomfort. It’s essential to follow their instructions carefully and taper off medicines as directed.
- Returning Home: Depending on your progress and comfort level, you can return home within a day, often with specific instructions for ongoing physical therapy and home care.
Recovery at Home: Essential Steps for Success
Following discharge, continued recovery at home is crucial:
- Physical Therapy: Regular physical therapy exercises are essential for regaining flexibility and reducing tightness in your plantar fascia. These exercises can be performed at home or in an outpatient physical therapy clinic, depending on your progress and the complexity of the surgery.
- Rest and Activity Balance: While rest is necessary for healing, gentle movement is crucial to prevent stiffness. As your body tolerates them, gentle calf stretches, and light activities like walking short distances are encouraged.
- Precautions: To prevent complications, avoid strenuous activities that could strain your foot, such as heavy lifting, prolonged standing, or high-impact exercises, until your doctor clears you.
- Pain Management: Continue taking pain medication as your doctor prescribes, gradually reducing it as your pain improves.
- Scar Management: If you have any scarring, your doctor may recommend scar massage techniques or silicone scar sheets to minimize their appearance.
Additional Considerations for a Successful Recovery Abroad
- Communication: Ensure clear communication with your doctor throughout the process, before and after you return home. Don’t hesitate to ask questions or voice concerns, especially if you’re recovering from surgery abroad.
- Follow-Up Care: Schedule appointments with your doctor or surgeon to monitor your progress and ensure proper healing. This may involve follow-up consultations in your home country or virtually with a doctor abroad.
Remember: Recovery from plantar fasciitis surgery is a gradual process. Be patient with yourself, listen to your body, and focus on following your doctor’s instructions and physical therapy routines. By following these guidelines and adhering to your recovery plan, you’ll be well on your way to enjoying pain-free heels and returning to your favorite activities.
What Are Some Risks and Complications of Plantar Fasciitis Surgery?
While minimally invasive plantar fasciitis surgery offers a permanent solution to heel pain, understanding the potential risks and complications is crucial, especially if you’re considering medical tourism. This article explores the risks associated with plantar fasciitis surgery abroad and emphasizes the importance of choosing a qualified surgeon to minimize these risks.
Common Complications
Bleeding and Infection: As with any surgery, bleeding and infection are potential risks after plantar fasciitis surgery. Bleeding can occur during or after surgery, and infection can develop if sterile techniques aren’t strictly followed. Choosing a board-certified podiatrist or foot and ankle surgeon at a JCI-accredited facility reduces these risks. Diligent adherence to post-operative care instructions is also essential. Open communication with your doctor throughout the process is crucial.
Swelling and Pain: Following plantar fasciitis surgery, swelling and bruising around the heel and incision site are common. The extent and duration of swelling will vary depending on the individual, but it typically subsides gradually over several weeks. Pain medication can help manage discomfort during this initial healing phase.
Scarring: Scarring is inevitable with any surgery, and plantar fasciitis surgery is no exception. However, skilled podiatrists or foot and ankle surgeons aim for minimal incisions and utilize techniques that minimize scar visibility. A proper scar care regimen is crucial for optimal healing and reducing scar prominence. Your surgeon might recommend silicone gel sheets or scar massage therapy.
Pain and Discomfort: Some discomfort and pain are expected after surgery, and your surgeon will prescribe medication to manage them effectively. The discomfort usually eases within the first few days or weeks as healing progresses.
Stiffness: After surgery, stiffness in the foot and ankle can occur, limiting your range of motion. Physical therapy is often recommended to regain flexibility and movement.
Uncommon Complications
Nerve Injury: Although nerve damage during surgery is uncommon, it can lead to numbness, tingling, or weakness in the foot.
Incomplete Plantar Fascia Release: In rare cases, the plantar fascia might not be adequately released during surgery, potentially leading to persistent heel pain. Revision surgery might be necessary to address this issue.
Complex Regional Pain Syndrome (CRPS): This rare condition, formerly known as Reflex Sympathetic Dystrophy (RSD), is characterized by chronic pain, swelling, and stiffness that can develop after surgery. There is no known cause, and treatment can be challenging.
Minimizing Risks and Optimizing Outcomes
Choosing a Qualified Surgeon: When considering plantar fasciitis surgery abroad, it is paramount to prioritize a board-certified podiatrist or foot and ankle surgeon with experience in minimally invasive procedures. Research the surgeon’s qualifications and the facility’s accreditation (look for JCI accreditation).
Open Communication: Discuss your expectations, potential risks of plantar fasciitis surgery, and any concerns with your doctor before surgery. Clear communication is even more critical if you’re recovering from surgery abroad.
Post-Operative Care: Diligently following your surgeon’s post-operative care instructions is crucial for a successful recovery and minimizes the risk of complications like infection.
Remember: While complications from plantar fasciitis surgery are uncommon, being informed empowers you to make informed decisions about your treatment plan. By choosing a qualified surgeon, openly communicating your concerns, and following post-operative care instructions, you can significantly reduce the risk of complications and optimize your journey toward a pain-free future.
Am I a Good Candidate for Plantar Fasciitis Surgery?
Plantar fasciitis, the inflammation of the plantar fascia tissue in your heel, can cause debilitating pain and disrupt your daily life. While minimally invasive plantar fasciitis surgery offers a permanent solution, it’s not always the first course of action. This self-assessment guide can help you determine if surgery might be the right option for you.
Severity of Symptoms
- Pain: Do you experience persistent, sharp pain in your heel, especially in the morning or after long periods of standing or walking? Does the pain worsen with activity and improve with rest
- Stiffness: Is there a noticeable stiffness or tightness in your heel, mainly when you first get out of bed in the morning?
- Limited Mobility: Does plantar fasciitis significantly limit your ability to participate in activities you enjoy, such as walking, running, or exercising?
Failure of Conservative Treatments
- Non-surgical Options: Have conservative treatments like rest, stretching exercises, physical therapy, orthotics, night splints, anti-inflammatory medication, or activity modification not provided adequate relief for your heel pain?
- Treatment Duration: Have you consistently tried conservative treatments for at least six months without significant improvement?
Impact on Daily Life
- Pain Disruption: Does the heel pain significantly disrupt your daily activities, work, or sleep?
- Lifestyle Limitations: Does plantar fasciitis significantly limit your ability to participate in activities you enjoy, such as walking, running, or standing for extended periods?
Seeking Professional Guidance
This self-assessment can be a helpful starting point, but consulting a board-certified podiatrist or foot and ankle surgeon is crucial for a definitive answer. Here’s what to expect during your consultation:
- Medical History Review: Your doctor will review your medical history, including any pre-existing conditions and medications you take.
- Physical Examination: Your foot, ankle, and range of motion will be assessed during a thorough physical examination. Your doctor will also press on the affected area to determine the severity of your pain.
- Imaging Tests: X-rays or imaging tests like ultrasound may be recommended to rule out other potential causes of heel pain, such as a stress fracture.
- Treatment Options Discussion: Your doctor will discuss the potential benefits and risks of plantar fasciitis surgery compared to other options, such as continued conservative treatments or alternative therapies.
Additional Considerations
- Recovery Timeline: Recovery time varies depending on the surgical approach and the severity of your plantar fasciitis. Following surgery, physical therapy may be recommended to regain strength and flexibility in your foot and ankle.
- Long-Term Management: While plantar fasciitis surgery can provide significant pain relief, proper footwear choices, stretching exercises, and activity modifications might still be necessary to prevent a recurrence.
Remember: Open communication with your doctor throughout the process is essential. Discuss your concerns about plantar fasciitis surgery and ensure you understand the potential benefits and risks. By carefully considering these factors and consulting with a qualified healthcare professional, you can determine if plantar fasciitis surgery is the best path to finally walk comfortably and pain-free again.
What Is Plantar Fasciitis Surgery?
Plantar fasciitis, the inflammation of the plantar fascia tissue in your heel, can cause significant pain and disrupt your daily life. While conservative treatments are often the first line of defense, minimally invasive plantar fasciitis surgery offers a permanent solution for those who haven’t found relief with other methods. This article explores the purpose and benefits of plantar fasciitis surgery.
Understanding Plantar Fasciitis
The plantar fascia is a thick band of tissue that runs along the bottom of your foot, connecting your heel to your toes and supporting the arch. Plantar fasciitis occurs when this tissue becomes inflamed or irritated, causing heel pain, especially in the morning or after long periods of standing or walking.
What is Plantar Fasciitis Surgery?
Plantar fasciitis surgery is a minimally invasive outpatient procedure designed to address the inflamed plantar fascia and alleviate heel pain. Here’s a simplified overview of the typical procedure:
- Anesthesia: Plantar fasciitis surgery is typically performed under local anesthesia with sedation, allowing you to remain awake and relaxed during the procedure. In some cases, general anesthesia might be used.
- Incision: The surgeon makes a small incision on the sole of your foot near the affected area. The size and location of the incision will depend on the specific surgical technique used.
- Fasciotomy: One of the most common techniques involves a fasciotomy, where the surgeon partially releases the plantar fascia to reduce tension and inflammation in the tissue.
- Endoscopic Surgery: In some cases, an endoscopic approach might be used. This minimally invasive technique utilizes a small camera and specialized instruments inserted through a tiny incision to perform the fasciotomy.
- Other Techniques: Depending on the severity of your plantar fasciitis, other procedures might be combined with a fasciotomy, such as removing a heel spur if present.
- Closure: The incision is then closed with stitches or surgical glue.
Benefits of Plantar Fasciitis Surgery
While conservative treatments like physical therapy and orthotics are often effective for plantar fasciitis, surgery offers a permanent solution for chronic pain that hasn’t responded to other methods. Here are some critical advantages of plantar fasciitis surgery:
- Pain Relief: The primary benefit is eliminating chronic heel pain associated with plantar fasciitis. This allows for pain-free walking, standing, and participation in various activities.
- Improved Function: Plantar fasciitis surgery can significantly improve your foot function and mobility by alleviating pain and inflammation. Activities like walking, running, and exercise become more manageable and enjoyable.
- Enhanced Quality of Life: Chronic pain from plantar fasciitis can significantly impact your daily life. Surgery can provide long-term pain relief and improve your overall quality of life.
- Faster Recovery: Minimally invasive techniques typically promote a quicker recovery compared to traditional open surgeries.
- Reduced Risk of Recurrence: Addressing the underlying cause of plantar fasciitis through surgery can significantly reduce the risk of future flare-ups.
Ankle Reconstruction
Our ankles are the workhorses of our bodies, silently providing stability and balance with every step. They propel us forward during walks, runs, and adventures, allowing us to explore the world with confidence. But for many Americans, ankle injuries or chronic conditions like arthritis can cause significant pain, instability, and limitations in mobility. Thankfully, minimally invasive ankle reconstruction surgery offers a solution to restore pain-free movement and get you back on your feet with renewed vigor.
Relief for Your Ankle Pain: A Surgical Solution
Ankle reconstruction surgery encompasses various procedures designed to address specific ankle problems. These procedures can address issues like ligament tears, cartilage damage, bone fractures, and deformity caused by arthritis. Here’s a closer look at the benefits of minimally invasive ankle reconstruction surgery:
- Reduced Pain and Discomfort: Surgery can significantly alleviate pain, inflammation, and stiffness in the ankle joint, allowing you to walk, stand, and participate in daily activities without discomfort.
- Improved Stability and Balance: Reconstruction surgery can repair damaged ligaments or correct bony deformities, enhancing stability and balance in the ankle joint. This reduces the risk of future sprains or injuries.
- Enhanced Range of Motion: By addressing issues that limit movement, ankle reconstruction surgery can significantly improve your range of motion in the ankle joint. This allows for more comfortable walking, running, and participation in physical activities.
- Faster Recovery: Minimally invasive techniques typically involve smaller incisions, less tissue disruption, and quicker recovery times than traditional open surgeries.
Medical Tourism: A Pathway to Affordable Care
The high cost of ankle reconstruction surgery in the US can often be a barrier to treatment. Medical tourism offers a compelling alternative, allowing access to high-quality surgery at a fraction of the typical US cost. Imagine waking up pain-free after ankle reconstruction surgery, followed by a relaxing recovery period in a new destination. Medical tourism lets you seamlessly blend the allure of travel with the expertise of board-certified orthopedic surgeons abroad, making it a strategic choice for regaining pain-free mobility.
How Much Can I Save?
The significant cost savings offered by medical tourism can be a driving factor for those considering ankle reconstruction surgery. Here’s a glimpse into the price disparity between the US and popular medical tourism destinations for ankle reconstruction surgery:
| Country | Estimated Range for Ankle Reconstruction Surgery (USD) | Important Note |
|---|---|---|
| United States | $15,000 - $50,000+ | Prices vary depending on the surgeon's experience, location, facility fees, anesthesia type, and complexity of the procedure. |
| Mexico | $8,000 - $18,000 | Consider travel and potential communication barriers. Research facility accreditations (like JCI) and surgeon qualifications. |
| Costa Rica | $9,000 - $20,000 | Similar considerations as Mexico regarding travel and communication. Focus on JCI-accredited facilities and board-certified surgeons. |
| Colombia | $7,000 - $16,000 | A popular choice, but thorough research is crucial. Ensure JCI accreditation and surgeon qualifications specializing in ankle reconstruction. |
| Thailand | $5,000 - $12,000 | It is a budget-friendly option, but significant research is necessary due to varying quality standards. Choose JCI-accredited facilities and board-certified surgeons with experience in ankle reconstruction. |
| India | $4,000 - $10,000 | The most comprehensive range is due to varying quality standards. Extensive research of facilities, surgeon credentials, and accreditations is essential. |
| Hungary | $8,000 - $16,000 | Offers a balance between affordability and quality care in Europe. Look for JCI accreditation and surgeon qualifications in ankle reconstruction. |
| Poland | $7,000 - $14,000 | Similar considerations as Hungary regarding affordability and quality. Research JCI accreditation and surgeon qualifications specializing in ankle reconstruction. |
| Czech Republic | $6,000 - $12,000 | Similar considerations as Hungary and Poland regarding affordability and quality. Research JCI accreditation and surgeon qualifications in ankle reconstruction. |
| Spain | $10,000 - $20,000 | Popular European destination with high-quality facilities. Research surgeon experience and facility accreditations, specifically for ankle reconstruction procedures. |
Please note: These are average costs and can vary depending on the surgeon’s experience, facility fees, the specific procedure (type of ankle reconstruction surgery needed), and post-surgical care needs. It’s crucial to get quotes directly from clinics you’re considering.
By carefully considering minimally invasive ankle reconstruction surgery and exploring medical tourism options, you can take the first step towards
Which Countries Specialize in Ankle Reconstruction Surgery?
Ankle injuries and chronic conditions like arthritis can significantly impact your mobility and quality of life. In the US, the high cost of minimally invasive ankle reconstruction surgery can be a barrier to regaining pain-free movement. Thankfully, medical tourism offers a compelling alternative – access to high-quality surgical procedures at a fraction of the typical US expense. However, prioritizing surgeon expertise and facility quality is crucial for successful outcomes.
Central and South America
- Costa Rica: Beyond its stunning rainforests and volcanoes, Costa Rica attracts medical tourists seeking affordable ankle reconstruction surgery. Costa Rican orthopedic surgeons are experienced in minimally invasive techniques, promoting faster recovery times. Affordability and proximity to the US make it a convenient option. Ensure Joint Commission International (JCI) accreditation for the facility and surgeon certification from the Costa Rican College of Surgeons (Colegio de Cirujanos y Dentistas de Costa Rica).
- Colombia: Emerging as a leader in medical tourism, Colombia offers ankle reconstruction surgery at significant cost savings compared to the US. Colombian orthopedic surgeons are increasingly skilled in minimally invasive techniques. Remember, thorough research is crucial. Look for JCI-accredited facilities and surgeons certified by the Colombian Society of Orthopaedics and Traumatology (Sociedad Colombiana de Ortopedia y Traumatología – SCOT).
Europe
- Czech Republic: This European nation is gaining recognition for its orthopedic surgery expertise. Czech surgeons experienced in minimally invasive ankle reconstruction procedures promote faster recovery times and minimal scarring. Look for JCI-accredited facilities and surgeons certified by the Czech Medical Chamber.
- Poland: Similar to the Czech Republic, Poland offers high-quality care at affordable prices. Polish orthopedic surgeons are well-versed in minimally invasive techniques, ensuring a faster return to an active life. Verify JCI accreditation for the facility and surgeon certification from the Polish Society of Orthopaedics and Traumatology (PTOiTr).
- Hungary: Offering a balance between affordability and quality care, Hungary attracts medical tourists seeking ankle reconstruction surgery. Hungarian orthopedic surgeons are increasingly experienced in minimally invasive techniques. Look for JCI-accredited facilities and surgeons certified by the Hungarian Society of Orthopaedics (Magyar Ortopédiai Társaság – MOT).
Asia
- India: A leader in medical tourism, India offers ankle reconstruction surgery at a significant cost savings compared to the US. While affordability is a draw, India boasts a growing pool of highly skilled orthopedic surgeons experienced in minimally invasive techniques. Remember, thorough research is crucial. Ensure JCI accreditation for the facility and surgeon certification from the National Board of Orthopaedics (NBO) or the Indian Orthopaedic Association (IOA).
- Thailand: A budget-friendly option, Thailand offers ankle reconstruction surgery at attractive prices. However, extensive research is necessary due to varying quality standards. Choose JCI-accredited facilities and surgeons certified by the Medical Council of Thailand and the Thai Orthopaedic Association.
Remember: While cost savings are a significant factor, prioritizing your health is paramount. Focus on JCI-accredited facilities and surgeons with board certification from your chosen destination’s relevant national orthopedic surgery association. By carefully researching your options, you can confidently embark on your journey to regaining pain-free mobility and an active lifestyle.
What Is the Recovery Process for Ankle Reconstruction Surgery?
Minimally invasive ankle reconstruction surgery offers a solution to chronic ankle pain and instability, but understanding the recovery process is crucial, especially if you’re considering medical tourism. This article explores the typical recovery timeline for ankle reconstruction surgery abroad and provides valuable tips to optimize your journey back to pain-free mobility.
Preparing for a Smooth Recovery
Even before your ankle reconstruction surgery abroad, proactive steps can ensure a smooth recovery:
- Pre-Operative Conditioning: Strengthen your calf and ankle muscles through exercises prescribed by your doctor or physical therapist. Stronger muscles will aid in a faster and more complete recovery after surgery.
- Post-Surgical Care Options: Discuss post-surgical care with your doctor. Some hospitals or clinics may offer rehabilitation packages tailored to ankle reconstruction recovery. Explore these options and inquire about the qualifications of the physical therapists involved.
- Packing Essentials: Pack comfortable, supportive shoes with good arch support and a wide toe box to accommodate post-surgical swelling. Consider bringing a compression stocking to manage swelling and a supportive brace for added stability, especially if recommended by your doctor.
The Ankle Reconstruction Surgery Recovery Timeline
- Hospital Stay: Following successful surgery, you can expect a short hospital stay, typically 1-3 days, depending on the complexity of the procedure and the facility’s protocols. Pain management and initial physical therapy will begin during this time.
- Physical Therapy: Physical therapy is a cornerstone of recovery and typically begins within a day or two after surgery. These exercises will focus on improving range of motion, reducing stiffness, and strengthening the muscles around your ankle joint. Physical therapy can continue for several weeks as an inpatient or outpatient, depending on your progress.
- Pain Management: Your doctor will prescribe pain medication to manage post-surgical discomfort. It’s essential to follow their instructions carefully and taper off medicines as directed.
- Returning Home: Depending on your progress and comfort level, you can return home within a few days, often with specific instructions for ongoing physical therapy and home care.
Recovery at Home: Essential Steps for Success
Following discharge, continued recovery at home is crucial:
- Physical Therapy: Regular physical therapy exercises are essential for regaining strength, flexibility, and balance in your ankle joint. These exercises can be performed at home or in an outpatient physical therapy clinic, depending on your progress and the complexity of the surgery.
- Rest and Activity Balance: While rest is necessary for healing, gentle movement is crucial to prevent stiffness and promote circulation. As tolerated, gentle ankle stretches, light walking with crutches or a walker, and low-impact exercises like swimming are encouraged.
- Precautions: To prevent complications, avoid strenuous activities that could strain your ankle, such as running, jumping, or heavy lifting, until your doctor clears you.
- Pain Management: Continue taking pain medication as your doctor prescribes, gradually reducing it as your pain improves.
- Scar Management: If you have any scarring, your doctor may recommend scar massage techniques or silicone scar sheets to minimize their appearance.
Additional Considerations for a Successful Recovery Abroad
- Communication: Ensure clear communication with your doctor throughout the process, before and after you return home. Don’t hesitate to ask questions or voice concerns, especially if you’re recovering from surgery abroad.
- Follow-Up Care: Schedule appointments with your doctor or surgeon to monitor your progress and ensure proper healing. This may involve follow-up consultations in your home country or virtually with a doctor abroad.
Remember: Recovery from ankle reconstruction surgery is a gradual process. Be patient with yourself, listen to your body, and focus on following your doctor’s instructions and physical therapy routines. By following these guidelines and adhering to your recovery plan, you’ll be well on your way to regaining pain-free mobility and getting back to the activities you enjoy.
What Are Some Potential Risks and Complications of Ankle Reconstruction Surgery?
Minimally invasive ankle reconstruction surgery offers a solution to chronic ankle pain and instability, but understanding the potential risks and complications is crucial, especially if you’re considering medical tourism. This article explores the risks associated with ankle reconstruction surgery abroad and emphasizes the importance of choosing a qualified surgeon to minimize these risks.
Common Complications
- Bleeding and Infection: As with any surgery, bleeding and infection are potential risks after ankle reconstruction surgery. Choosing a board-certified orthopedic surgeon at a JCI-accredited facility significantly reduces these risks. Strict adherence to sterile techniques during surgery and diligent follow-through with post-operative care instructions are essential. Open communication with your doctor throughout the process is crucial to address any concerns promptly.
- Swelling and Bruising: Following ankle reconstruction surgery, swelling and bruising around the ankle and incision site are common. The extent and duration of swelling will vary depending on the individual and the complexity of the procedure, but it typically subsides gradually over several weeks. Pain medication can help manage discomfort during this initial healing phase.
- Scarring: Scarring is inevitable with any surgery, and ankle reconstruction surgery is no exception. However, skilled orthopedic surgeons aim for minimal incisions and utilize techniques that minimize scar visibility. A proper scar care regimen is crucial for optimal healing and reducing scar prominence. Your surgeon might recommend silicone gel sheets or scar massage therapy.
- Pain and Discomfort: Some discomfort and pain are expected after surgery, and your surgeon will prescribe medication to manage them effectively. The discomfort usually eases within the first few days or weeks as healing progresses.
- Stiffness: After surgery, stiffness in the ankle joint can occur, limiting your range of motion. Physical therapy is a cornerstone of recovery and is crucial for regaining flexibility and movement.
Uncommon Complications
Nerve Injury: Although nerve damage during surgery is uncommon, it can lead to numbness, tingling, or weakness in the foot or toes.
Incomplete Ligament Repair or Bone Realignment: In rare cases, ligaments might not be adequately repaired or bone fragments might not be perfectly realigned during surgery. This could lead to persistent instability or pain, potentially requiring revision surgery.
Complex Regional Pain Syndrome (CRPS): This rare condition, formerly known as Reflex Sympathetic Dystrophy (RSD), is characterized by chronic pain, swelling, and stiffness that can develop after surgery. There is no known cause, and treatment can be challenging.
Minimizing Risks for a Successful Recovery
Choosing a Qualified Surgeon: When considering ankle reconstruction surgery abroad, prioritizing a board-certified orthopedic surgeon with experience in minimally invasive ankle procedures is paramount. Research the surgeon’s qualifications, including certifications and experience with your specific condition. Look for a surgeon affiliated with a JCI-accredited facility.
Open Communication: Discuss your expectations, potential risks of ankle reconstruction surgery, and any concerns with your doctor before surgery. Clear communication is even more critical if you’re recovering from surgery abroad. Don’t hesitate to ask questions and voice any anxieties you may have.
Post-Operative Care: Diligently following your surgeon’s post-operative care instructions is crucial for a successful recovery and minimizes the risk of complications like infection. This may include proper wound care, weight-bearing limitations, medication adherence, and attending physical therapy sessions.
Follow-Up Care: Schedule appointments with your doctor or surgeon to monitor your progress and ensure proper healing. This may involve follow-up consultations in your home country or virtually with a doctor abroad.
Remember: While complications from ankle reconstruction surgery are uncommon, being informed empowers you to make informed decisions about your treatment plan. By choosing a qualified surgeon, openly communicating your concerns, and following post-operative care instructions, you can significantly reduce the risk of complications and optimize your journey back to pain-free mobility.
Am I a Good Candidate for Ankle Reconstruction Surgery?
Chronic ankle pain and instability caused by injuries or conditions like arthritis can significantly impact your mobility and quality of life. While minimally invasive ankle reconstruction surgery offers a solution, it’s not always the first course of action. This self-assessment guide can help you determine if surgery might be the right option for you.
- Severity of Your Symptoms
- Failure of Conservative Treatments
- Impact on Daily Life
- Seeking Professional Guidance
- Pain: Do you experience persistent pain, swelling, or instability in your ankle, especially after activity or prolonged standing? Does the pain limit your ability to walk comfortably?
- Instability: Does your ankle feel weak or give way easily, increasing your risk of falls?
- Stiffness: Is there a noticeable stiffness or tightness in your ankle joint, limiting your range of motion?
- Non-surgical Options: Have conservative treatments like rest, physical therapy, bracing, anti-inflammatory medication, activity modification, or injections not provided adequate relief for your pain and instability?
- Treatment Duration: Have you consistently tried conservative treatments for at least six months without significant improvement?
- Activity Limitations: Does your ankle pain and instability significantly limit your ability to participate in activities you enjoy, such as walking, running, exercising, or work that requires physical mobility?
- Quality of Life: Does your ankle condition significantly disrupt your daily life, causing difficulty with tasks like walking up stairs or uneven surfaces?
This self-assessment can be a helpful starting point, but consulting a board-certified orthopedic surgeon specializing in ankle disorders is crucial for a definitive answer. Here’s what to expect during your consultation:
- Medical History Review: Your doctor will review your medical history, including any pre-existing conditions and medications you take.
- Physical Examination: A thorough physical examination will assess your ankle joint, range of motion, stability, and any tenderness or swelling.
- Imaging Tests: X-rays, MRI scans, or other imaging tests may be recommended to diagnose the cause of your ankle pain and instability, such as ligament tears, cartilage damage, or bone fractures.
- Treatment Options Discussion: Your doctor will discuss the potential benefits and risks of ankle reconstruction surgery compared to other options, such as continued conservative treatments or alternative therapies.
Additional Considerations
- Recovery Timeline: Recovery from ankle reconstruction surgery can vary depending on the specific procedure and the severity of your condition. Physical therapy will be crucial for regaining strength, flexibility, and stability in your ankle joint.
- Long-Term Management: While ankle reconstruction surgery can restore stability and reduce pain, proper footwear choices, regular physical therapy exercises, and activity modifications might still be necessary to maintain long-term joint health.
Remember: Open communication with your doctor throughout the process is essential. Discuss your concerns about ankle reconstruction surgery and ensure you understand the potential benefits and risks. By carefully considering these factors and consulting with a qualified orthopedic surgeon, you can determine if ankle reconstruction surgery is the best path to regain pain-free mobility and get back to the activities you enjoy.
What Is Ankle Reconstruction Surgery?
Chronic ankle pain and instability caused by injuries or conditions like arthritis can significantly impact your mobility and quality of life. While conservative treatments like physical therapy and bracing are often the first line of defense, minimally invasive ankle reconstruction surgery offers a solution for those who haven’t found relief with other methods. This article explores the purpose and benefits of ankle reconstruction surgery.
Understanding Ankle Anatomy
Your ankle joint is a complex structure where the shinbone (tibia) and fibula (calf bone) meet the talus bone of your foot. Ligaments, strong bands of tissue, stabilize the joint and allow for movement. Cartilage provides cushioning between the bones.
What is Ankle Reconstruction Surgery?
Ankle reconstruction surgery is a minimally invasive outpatient procedure designed to address instability, pain, or deformity in the ankle joint. There are various surgical approaches depending on the specific issue:
- Arthroscopy: A small camera is inserted through a tiny incision to visualize the joint and perform repairs like trimming damaged cartilage or removing bone fragments.
- Ligament Repair: Torn or stretched ligaments are repaired or reconstructed using sutures or anchors to restore stability.
- Tendon Transfers: In some cases, tendons from other parts of the foot might be used to reinforce weakened ligaments.
- Bone Procedures: Fractures or bone misalignments might require procedures like bone grafting or osteotomy (cutting and repositioning bone) to correct the deformity.
Benefits of Ankle Reconstruction Surgery
While conservative treatments are often attempted first, ankle reconstruction surgery offers a solution for those who haven’t found relief and continue to experience:
- Pain Relief: Surgery aims to eliminate chronic ankle pain caused by instability, arthritis, or other conditions. This allows for pain-free movement and participation in various activities.
- Improved Stability: By repairing or reconstructing ligaments or addressing other structural issues, surgery can significantly improve ankle joint stability, reducing the risk of sprains and falls.
- Enhanced Mobility: Improved stability and reduced pain can significantly enhance your ankle’s range of motion, allowing for more comfortable walking, running, and participation in physical activities.
- Increased Quality of Life: Chronic ankle pain and instability can significantly impact your daily life. Surgery can provide long-term pain relief and improved joint function, enhancing your overall quality of life.
- Faster Recovery: Minimally invasive techniques typically promote a quicker recovery compared to traditional open surgeries.
Remember: Ankle reconstruction surgery is a personalized procedure. Consulting with a board-certified orthopedic surgeon specializing in ankle disorders is crucial to determine if surgery is the right option for you and discuss the most suitable surgical approach for your specific condition.
